
Introduction
The Set Point Theory of weight regulation is an attempt to explain why people can maintain their body weight at a relatively stable level for long periods. The Set Point Theory suggests that body weight is regulated by a feedback control mechanism in order to maintain a set body weight, often times one that is “predetermined” (1).
I want to lay my hypothesis out from the very beginning of this article and then work through the different data points, ideas, and observations that support this hypothesis. I will also point toward data that might “break” my hypothesis as I want to also use this as an exercise in working through my hypothesis and exposing weak points.
Formally, here it is: the human body has myriad adaptive mechanisms that work orthogonally and synergistically that protect against energy imbalance; however, these mechanisms are often overpowered and unable to compensate to powerful external stimuli/signals. Furthermore, different adaptations in different tissues matter substantially in how a set point manifests itself.
More informally, I find that the Set Point Theory of weight regulation is limited to a narrow bandwidth and, for all intents and purposes, fails to manifest itself in meaningful ways in most people living in the current environment due to the magnitude and duration of signals being sent to the human body.
Now, let me work through the first part of the hypothesis: the human body has myriad adaptive mechanisms that work orthogonally and synergistically that protect against weight gain and weight loss.
Reasons Set Point is a Real Thing
Time to plant the first flag. Adaptive mechanisms that defend against weight loss, specifically as it relates to energy balance and fat mass do exist.
There is substantial data to support the idea that there are mechanisms by which the human body regulates energy intake and expenditure in order to maintain homeostasis and keep body weight, and specifically body fat mass stable over fairly long periods. I want to highlight many of these mechanisms through examples to motivate the idea.
Adaptations to Energy Loss
Most studies that attempt to modulate energy intake and expenditure and examine how the body responds are unable to intervene in humans without making the intervention perceptible to the participants. However, recent studies have utilized a novel approach to tease out some interesting observations.
Recently, two papers published by Ferrannini et al. and Polidori et al.were able to quantify an adaptive response in food intake that offset a pharmacologically induced increase in calorie expenditure via an unconventional method, spilling extra glucose into the urine.
The recent anti-hypergylcemic drugs, SGLT-2 inhibitors, lower blood glucose by decreasing the rate of glucose resorption in the kidneys of people with diabetes. This results in a roughly 200 calorie per day loss that the participants are unaware of, the spilling of glucose simply removes 200 calories a day of chemical energy from the body. This leads to an initial weight loss of 6-10 pounds, which stabilizes overtime and eventually the weight loss stalls.
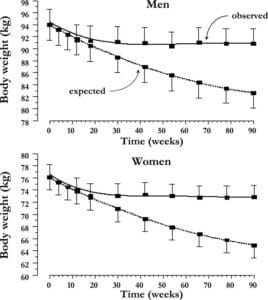
In the two aforementioned papers, the authors were able to track food consumption (energy intake) and energy expenditure. In their papers, the authors demonstrated that in both the short term, and the long term, this 200 calorie energy loss is offset by an increase in energy intake by 200 calories. This increase in energy intake is largely explained by increases in hunger. However, the initial 6-10 pound loss persists. This seems to indicate an adaptation for energy balance, not body mass per se. Which matters quite a bit when we consider the overall context of the idea of Set Point.
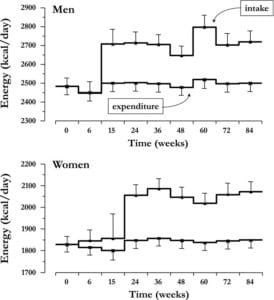
These data support the idea that the body has adaptive mechanisms that mitigate changes in energy expenditure in attempts to defend a current body weight, primarily due to a need for maintaining energy balance. However, it does not appear to, at least in this data, contribute largely to a rebound (these studies were short term and could not adequately assess this aspect of the hypothesis)
The Fat Thermostat
The data from the Canagliflozin studies (SGLT-2 inhibitors) above demonstrate the subtle, but effective, adaptive mechanisms the body has in place to defend against an energy imbalance. In addition to this, there are adaptive mechanisms that defend against changes in fat mass.
In mammals, including humans, there is a hormonal axis that helps regulate body fat mass in a way that attempts to keep fat mass within a narrow band. How narrow that band has not yet been elucidated and is speculation on my part at this point (more on this later in the article). This is called the adipostat and can be thought of as the Fat Thermostat. In its most simple form, it works with simple feedback loops.
Your fat mass produces a hormone known as leptin. In theory, as fat mass increases your leptin levels increase. This then sends a signal to the brain (specifically, the hypothalamic paraventricular nucleus) that ‘tells’ you to eat less, move more, and increase thermogenesis. When fat mass gets low and leptin levels drop, your brain gets signals to increase food intake and decrease activity.
The power of leptin can be observed in mice that are leptin-deficient or humans that are leptin-deficient. These mice, and humans, exhibit an extremely obese phenotype; it can be reversed with exogenous leptin. These data support the idea of mechanisms to maintain body fat.
This is a superficial introduction and we will discuss exactly where this breaks down later in the article.
I (don’t) Like to Move It, Move It
The work of Rudolph Leibel has been illuminating in demonstrating one of the key “adaptation” mechanisms that occurs to prevent weight loss or weight gain in humans. His work identified the role of physical activity, specifically non-exercise activity thermogenesis (NEAT). NEAT is essentially the caloric expenditure that occurs in a given day as a result of unstructured, often non-intentional physical activity.
Total body metabolism, which is commonly referred to as total energy expenditure, is the sum of your basal metabolic rate (BMR; also known as resting energy expenditure), exercise activity, thermic effect of food, and NEAT. In a series of studies (2, 3, 4), Dr. Leibel set out to understand the role of BMR and changes in NEAT and how they explain weight change in people, specifically among people who lost large amounts of weight and then gained it back. In these studies, Dr Leibel was able to pinpoint a few things: 1) with weight loss BMR does decrease and this does have a small impact on weight loss, but was not a robust effect or highly reproducible across studies; furthermore, it did not really explain much of the difference between people who regained lost weight and those who did not, 2) reductions in NEAT were a much bigger factor to weight regain and did explain much of the difference between people who regained lost weight and those who didn’t.
These data point to the fact that NEAT is a mechanism by which the body can defend against weight rebound. NEAT, while in some cases is controlled in an autonomic fashion, is more substantially controlled by overall lifestyle and deliberate action in the current, modern environment.
Dieting Trials
Weight rebound is an inherent aspect of dieting for most people, especially in people who have been engaged in randomized-controlled diets examining the efficacy of weight loss. For example, in a 10-year follow-up trial of the Diabetes Prevention Program, weight rebound was basically universal, with both lifestyle and metformin interventions showing weight rebound (4).
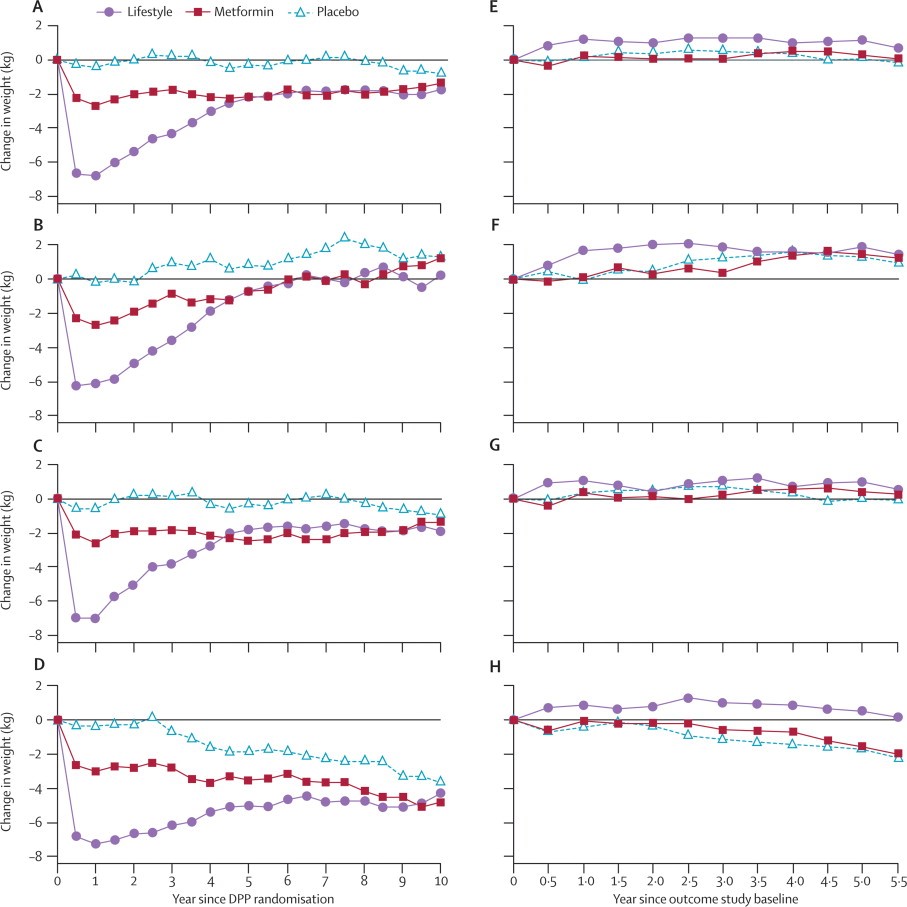
While much of this may be attributable to lack of adherence over time, there is also evidence that there is a change in metabolic rate that accompanies weight loss that can contribute to weigh regain. In a series of papers, Kevin Hall’s lab demonstrated that after substantial weight loss in the Biggest Loser challenge, most participants regained weight, with an average regain of ~30 kg over about 5.5 years. This coincided with a reduction in RMR of about 600 kcal/day at the end of the initial weight loss phase (5). However, their data indicated that this change in RMR was not correlated with the “weight rebound observed”.
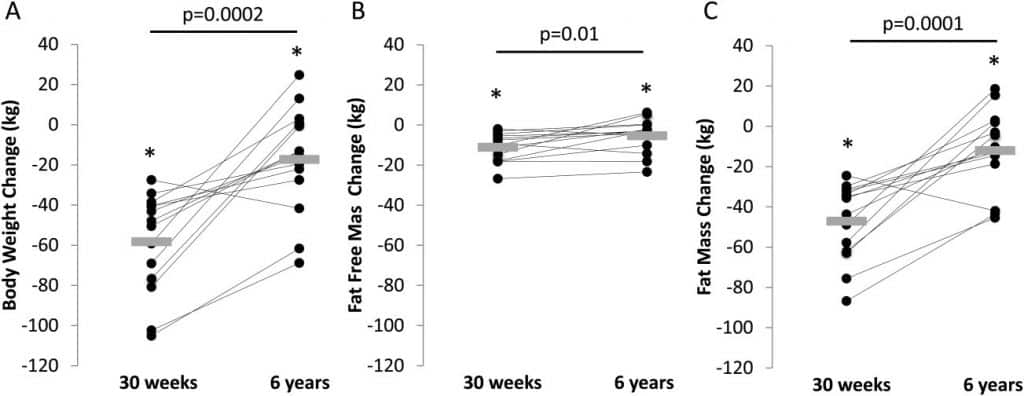
Set Point Failure Points
Our body has evolutionarily developed and conserved systems that are designed to maintain body weight and these mechanisms appear to have meaningful effects on the human body. However, there are some key areas that need to be considered when we think about these adaptive mechanisms and where they break down.
Set Point Mechanisms Just Are Not Powerful Enough
Earlier in the article, we mentioned the adipostat and its role in regulating fat mass. We have powerful epidemiological data to support the idea that the adipostat does not defend against obesity and maintaining a set body fat. Obesity rates have climbed over the past 100 years and it follows a fairly typical pattern, in lock-step with industrialization and moving from a developing country to a developed country. Look at the obesity trends and growth of the United States, Mexico, India, and China over the last 100 years. The data clearly show fat mass is increasing, despite the clear biology of leptin and the adipostat (I will provide an answer to this in the later sections)
Epidemiology data is hypothesis-generating, interventional data must bolster those data. Data from intervention trials in humans, specifically in obesity trials with leptin therapy, suggest that the leptin story is much more complicated than a simple thermostat in real life. While this mechanism can and does help maintain body fat levels in many mammals, this mechanism does not appear to be robust enough to really maintain or “adjust” body fat levels in humans.
In humans with no genetic leptin deficiency, administration of exogenous leptin (to activate the leptin signaling circuits) does not lead to robust or meaningful weight loss in humans. See here for a very nice, thorough review. The leptin resistance appears to be secondary and resultant from similar biological processes that create insulin resistance (e.g. obesity and inflammation). In this case, the adaptive mechanisms that exists to create a “set point” for body fat mass in humans are not robust enough to maintain a set body fat amidst strong external signals (again, more on this in coming sections).
Based on the past several decades and current trajectory of overweight and obesity rates it has hard to state the Set Point Theory is a collection of mechanisms powerful enough to maintain body weight in the current environment, it appears as though these Set Point mechanisms have likely met there match.
Too Much, or Too Long
One thing appears abundantly clear, the adaptive mechanisms in the body that maintain body weight operate in a narrow band. Many of the adaptive mechanisms work within the confines of human behavior: the increased hunger and food intake from the Canagliflozin trials support this.
However, as we can see from the changing human phenotype, these mechanisms are constrained in how powerful they can be. It appears that if signals are sufficiently large, and/or sufficiently long, they can “overpower” the adaptive mechanisms the body has in place and it is abundantly clear that the stimuli pressed upon humans is currently overwhelming these mechanisms and our ability to defend a lower set point is compromised.

The main stimuli that are responsible for the rise in body mass are, in my best approximation, lack of physical activity and increases in food intake.
In developed and developing countries occupational, recreational, and non-structured physical activity has declining to a substantial degree over the last 50-70 years. To put some numbers to this, the total percentage of jobs in the United States that are classified as “moderate physical activity” has dropped from just under 50% in 1960 to under 20% by 2010. The total percentage of sedentary jobs has risen from about 15% to 24%. For both men and women the total job related daily energy expenditure has decreased almost 200 calories per day since 1960 (6).
In American, the daily energy intake per person has increased ~350 kcal/day for children and ~500 kcal/day for adults based one study (7).
The reduction in activity may be more important than the increase in calories as we know that the type of stimuli and adaptation that comes from exercise matters a great deal (more on this in the next section).
When we hold these two data points in juxtaposition, it becomes very clear that our built environment, socio-cultural value structures, and modern way of life are clearly throwing a larger and more sustain signal than our adaptive mechanisms can handle.
Quality Matters in Biology
When thinking of set point it is much better to think about it as a dynamic changing point on the scale and more to do with a level of adiposity, which means to say that it isn’t really a point about weight* and more about adiposity. To put this in context, consider the adaptation that occurs to muscle mass over a lifetime. If the Set Point hypothesis about a specific body weight only were correct, then the growth and maintenance of skeletal muscle mass in adults would be much more rare and difficult to achieve than it is.
In most adult humans, adding 2-10kg of muscle mass over a 5-20 year period is not a difficult feat. This can be accomplished with fairly moderate but consistent interventions (e.g. engaging in resistance training and eating and adequate amount of protein). Fairly decent amounts of muscle tissue can be added in much shorter time frames. For example, in the seminal Bhasin 1996 study, healthy, young males increased fat free mass roughly 4.4 lbs (2 kg) over a 10 week resistance training intervention (8).
Additionally, one of the more common things we see is that women who have become pregnant and give birth to children often have the goal of returning to their initial body weight. In many cases women may gain ~2-4 pounds of lean mass during pregnancy (this means net accretion of muscle, bone, and/or organ tissue) (9). Thus a shifted new set point based on a new higher lean mass number.
To bring this back to the first point in this section, it is more likely that the adaptive mechanisms we have observed are more likely related to fat mass and overall energy balance than they are a specific scale weight*.
Energy Balance vs Mass Balance
Energy balance and mass balance are inextricably related and a positive energy balance leads to a positive mass balance, and vice versa. However, the type of mass balance change appears to matter in that fat mass accumulation and muscle mass accumulation (or bone mass) are often regulated by different stimuli and signals. The type of tissue that changes appears to have differential impacts on the overall body weight set point.
Closing Thoughts
There are adaptive mechanisms in the human body (and other mammalian species and maybe even non-mammalian species) that defend against energy imbalance, and as a consequence, changes in body mass. Outside of some limited investigations the vast preponderance of evidence indicates that there are adaptive mechanisms that attempt to “coerce” the body into a state of energy balance. These coercive mechanisms appear to operate within a limited scope and sufficiently large, and/or sufficiently long, signals are likely to override these systems. Those changes in body mass are dependent on the type of stimuli given, which can have substantially different impacts on the set point of body mass
*Here is a recent paper that directly contradicts my statement here and the data is interesting but I am not fully convinced based on this data. There are some issues here. Hat tip to Eric Trexler for sending me this paper and our discussions about it
**Special thanks to Zad Chow for his thoughts, comments, edits, and insights into this piece.
